There are many “facts” or pieces of common knowledge that we take at face value. Like that bulls hate the color red or goldfish have a 3‑second memory. In reality, these aren’t facts at all — just myths that get repeated over and over.
When it comes to bulls and goldfish, these myths probably aren’t harming anyone. But when it comes to medical conditions, myths can have a significant impact on someone’s physical or mental health.
Skin conditions in particular are often surrounded by misinformation — especially psoriasis. Unlearning some of what we know is a necessary step in decreasing stigma and helping people live healthier, happier lives.
August is Psoriasis Awareness Month, and psoriasis is one condition that has many myths around it. Here are 5 things you might think you know about psoriasis that are actually myths.
Myth 1: You Can “Catch” Psoriasis
Unlike the common cold or the flu, psoriasis is not something that can be passed from person to person. Psoriasis is not contagious, and you will not get psoriasis from interacting with someone who has it or from skin-to-skin contact.
Psoriasis is actually an autoimmune disease, which means that it is caused when your body has an overactive immune system and begins to attack other parts of your body, like tissue (such as skin). This attack shows up when your body creates new skin cells too quickly, causing them to form thick, scaly patches on your skin.
If you have any of these symptoms or suspect that you might have psoriasis, reach out to your Duly Health And Care dermatologist.
Myth 2: If You Have Psoriasis, It’s Your “Fault”
These thick, scaly patches of skin are called “plaques,” and they are not your fault. Contrary to some popular beliefs, psoriasis is not caused by bad hygiene. Psoriasis is thought to be passed through families and to have a genetic component.
While there is nothing you did to cause your psoriasis, it can be helpful to think about the factors that might be leading to flare-ups or making your symptoms worse.
Common Psoriasis Triggers
Different environmental or emotional factors can make your psoriasis worse — these are called “triggers.” Some common psoriasis triggers include:
- Stress
- Weather (either cold OR warm)
- Injury or illness
- Smoking or drinking
- Shaving
- Piercings or tattoos
To help manage triggers, keep track of the events that occur surrounding a flare-up. Was something stressful happening at work, or was there a change in the weather? After recording your observations, bring them to your Duly dermatologist to figure out your next steps.
Myth 3: There’s Only One Kind of Psoriasis
There are many different types of psoriasis, and they all show up on the skin a little differently:
- Plaque psoriasis is the most common psoriasis, affecting between 80% to 90% of psoriasis patients. Plaque psoriasis looks like silver, thick, raised patches of skin that often form on the elbows, knees, back, or scalp.
- Guttate psoriasis is the form of psoriasis that most often affects children. Unlike other forms of psoriasis, it often appears as little, scaly spots.
- Nail psoriasis can form alongside any other type of psoriasis. It can look like your nails pitting, crumbling, separating from the skin, or forming yellow/brown spots.
- Pustular psoriasis is a rarer form of psoriasis and it often occurs on the hand and feet in the form of scaly skin and blisters that are painful and pus-filled.
No two cases of psoriasis are exactly the same, and other forms of psoriasis will also show up differently than the ones listed above. For a complete list of different types of psoriasis — and what they look like — visit the American Academy of Dermatologists’ photo gallery.
Myth 4: Psoriasis Only Affects Your Skin
Some people might think that psoriasis is just a skin condition — and that it only causes cosmetic or surface-level discomfort for those who have it. This couldn’t be farther from the truth.
Psoriasis is a disease that can impact all aspects of a person’s life — from their social and romantic interactions to their general mental and physical health. Psoriasis is often associated with comorbidities, which is when someone has two or more diseases or health conditions at the same time.
Some common comorbidities that are seen when someone has psoriasis are:
- Arthritis
- Depression
- Cardiovascular diseases
- Inflammatory Bowel Syndrome (IBS)
Managing comorbidities is a key part of managing your psoriasis — and health in general. That’s why it’s so important to schedule and attend your annual wellness visit.
Myth 5: If You Have Psoriasis, There’s Nothing You Can Do About It
While there is no “cure” for psoriasis, there are many different kinds of treatment that can help you manage or decrease your symptoms.
At Duly, our dermatologists can help you develop a treatment plan to address your psoriasis that might include:
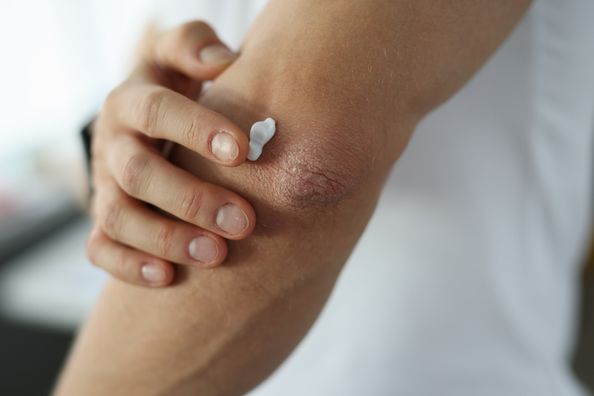
- Topical treatments: Creams, lotions, or ointments that you apply to your skin
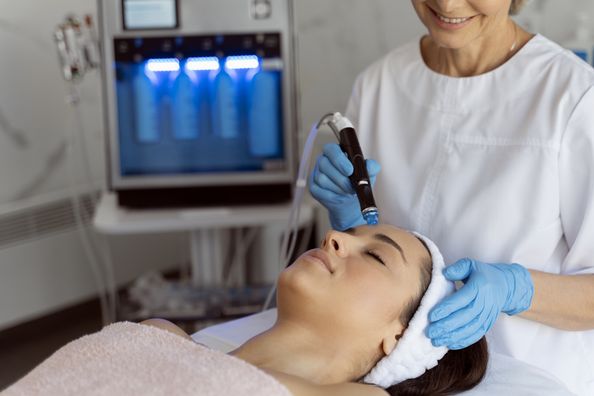
- Phototherapy: Appointments with your dermatologist where you undergo exposure to ultraviolet (UV) light under medical supervision (not the same (and safer) than just going to a tanning salon)
- Systemic medications: Prescription drugs that can be injected or taken orally
Together, We Can Treat Your Psoriasis
At Duly, our team of dermatologists can diagnose and treat your psoriasis. We will work to understand your condition, how it’s affecting your day-to-day life, and provide resources to help manage triggers and flare-ups.
While psoriasis is a condition that is surrounded by a lot of misinformation, we can change how people view and respond to it. By addressing common myths, we can help reduce the stigma that comes with psoriasis and create a better future for those living with it.
If you have symptoms or questions about psoriasis, reach out to your Duly Health And Care primary care provider, or find a dermatologist near you.
Health Topics: